How to Start Testosterone Replacement Therapy: 6-Step Guide 2025

Outcome: This guide provides a comprehensive roadmap for determining whether Testosterone Replacement Therapy (TRT) is right for you and how to begin treatment safely. Within 8-12 weeks of starting TRT, most men experience improved energy, mood, and physical performance. Skill level required: Beginner. Expected time commitment: 2-4 weeks for initial evaluation and treatment initiation.
What Is Testosterone Replacement Therapy and How Does It Work?
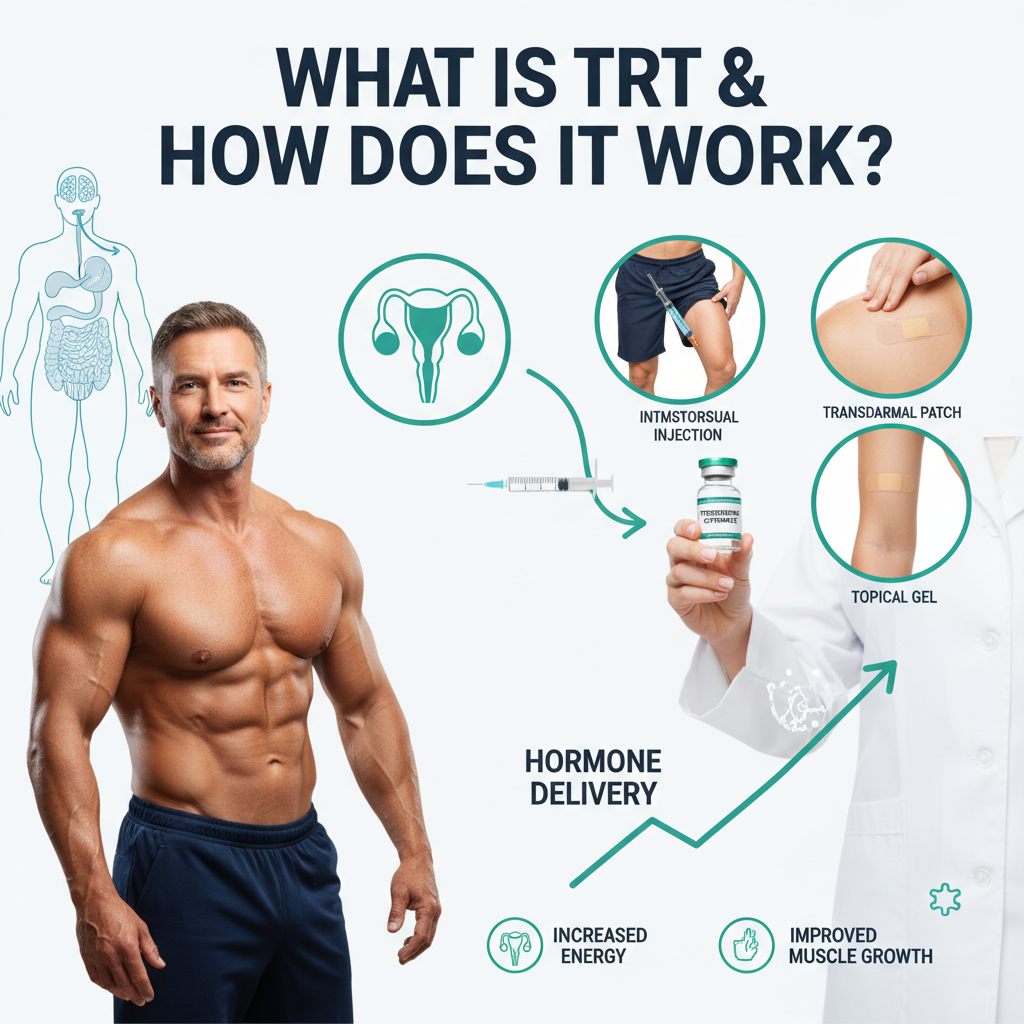
Testosterone Replacement Therapy (TRT) is a medical treatment designed to restore testosterone levels in men with clinically diagnosed hypogonadism or testosterone deficiency. According to the FDA (2023), TRT delivers synthetic testosterone or bioidentical hormones to supplement the body’s natural testosterone production when the testes, pituitary gland, or hypothalamus fail to produce adequate amounts of this essential androgen.
The treatment works by replacing deficient testosterone levels through various delivery methods including intramuscular injection, subcutaneous injection, transdermal application, testosterone gel, testosterone patch, or testosterone pellet implantation. TRT addresses symptoms of low testosterone including reduced libido, fatigue, muscle loss, mood changes, and decreased bone density. Male hormone therapy typically produces measurable improvements in serum testosterone levels within 2-4 weeks, with full symptom relief occurring at 8-12 weeks.
Before You Begin: Prerequisites
- Schedule appointment with primary care physician or endocrinologist
- Obtain comprehensive blood test measuring Total Testosterone, Free Testosterone, and bioavailable testosterone
- Verify testosterone levels below 300 ng/dL on two separate morning tests
- Complete prostate specific antigen (PSA) screening and complete blood count (CBC)
- Document low T symptoms for at least 3 months
- Verify insurance coverage or budget for out-of-pocket costs ($100-$500 monthly)
- Ensure no contraindications including prostate cancer, severe sleep apnea, or uncontrolled heart failure
Step 1: Recognize Signs You Need Testosterone Replacement Therapy

Identify whether you experience multiple symptoms of low testosterone requiring TRT. Common signs you need testosterone replacement therapy include persistent fatigue despite adequate sleep, decreased muscle mass, increased body fat (particularly abdominal), reduced libido, erectile dysfunction, mood disturbances including depression or irritability, difficulty concentrating, and decreased bone density.
Track your symptoms for 4-8 weeks using a daily journal. Note severity on a scale of 1-10. Men over 40 naturally experience age-related testosterone decline at approximately 1-2% annually, but this differs from clinical hypogonadism. Andropause or male menopause occurs gradually, whereas testosterone deficiency produces more severe symptoms requiring medical intervention.
Action items:
- Document all symptoms with duration and severity
- Eliminate other potential causes (sleep disorders, thyroid issues, vitamin D deficiency)
- Compare symptoms against validated screening tools like the ADAM questionnaire
- Schedule initial consultation if experiencing 3+ persistent symptoms
Step 2: Complete Comprehensive Testosterone Testing and Lab Results
Obtain baseline blood work for testosterone therapy between 7-11 AM when testosterone levels peak naturally. Your hormone doctor will order multiple tests to establish a complete hormonal profile and rule out other endocrine system disorders.
Essential lab tests needed before starting TRT:
| Test | Purpose | Normal Range |
|---|---|---|
| Total Testosterone | Measures combined free and bound testosterone | 300-1000 ng/dL |
| Free Testosterone | Measures bioactive unbound testosterone | 9-30 ng/dL |
| Sex Hormone Binding Globulin (SHBG) | Determines how much testosterone is bound | 10-57 nmol/L |
| Luteinizing Hormone (LH) | Evaluates pituitary gland function | 1.7-8.6 mIU/mL |
| Follicle Stimulating Hormone (FSH) | Assesses testicular function and fertility | 1.5-12.4 mIU/mL |
| Prostate Specific Antigen (PSA) | Screens for prostate issues | <4.0 ng/mL |
| Complete Blood Count (CBC) | Evaluates red blood cell production | Varies by component |
| Estrogen (Estradiol) | Monitors testosterone conversion to estrogen | 10-40 pg/mL |
Request a second confirmatory blood test 2-4 weeks after initial testing. According to clinical guidelines (Endocrine Society, 2018), diagnosis of hypogonadism requires two separate testosterone measurements below 300 ng/dL accompanied by symptoms.
Step 3: Consult Specialists to Determine If You’re a Good Candidate for TRT
Schedule consultations with qualified medical professionals specializing in hormone replacement therapy men. An endocrinologist specializes in endocrine treatment and hormonal health, while a urologist addresses male-specific reproductive and hormonal issues.
During your consultation, discuss whether testosterone replacement therapy is right for me based on your lab results testosterone, medical history, and symptoms. Your doctor will evaluate contraindications including active prostate cancer, breast cancer, severe obstructive sleep apnea, uncontrolled heart failure, or elevated hematocrit above 54%.
Questions to ask your hormone doctor:
- What are the benefits and risks of testosterone replacement therapy for my specific situation?
- How long does TRT take to work for symptom improvement?
- What does TRT do to your body in terms of metabolic changes?
- Does insurance cover testosterone replacement therapy or what is the out-of-pocket cost?
- How effective is testosterone replacement therapy compared to alternative treatments?
- Can TRT cause prostate cancer or other serious side effects?
- Does testosterone replacement therapy affect fertility and sperm count?
- Can you have children while on TRT or should I consider fertility preservation?
Verify your provider’s credentials and experience with TRT treatment programs. Reputable testosterone clinic physicians should be board-certified in endocrinology, urology, or internal medicine with specific training in male hormone replacement.
Step 4: Choose Your Testosterone Replacement Therapy Delivery Method
Select the optimal testosterone administration method based on lifestyle, convenience, cost, and symptom control. Each delivery system offers distinct advantages for testosterone replacement options.
Testosterone Injections (Most Common)
Intramuscular testosterone using testosterone cypionate or testosterone enanthate involves injecting into the gluteal or thigh muscle every 1-2 weeks. Injectable testosterone provides consistent hormone levels and costs $30-$100 monthly.
Subcutaneous testosterone uses smaller needles injected into abdominal fat 1-3 times weekly, producing more stable testosterone blood work results with fewer peak-and-trough fluctuations.
Pros: Cost-effective, reliable absorption, adjustable dosing
Cons: Requires injections, potential injection site discomfort, how often do you need testosterone injections (weekly or biweekly)
Testosterone Gel and Topical Testosterone
Products like AndroGel and Testim deliver testosterone through transdermal testosterone application daily. Testosterone cream absorbs through skin, providing steady hormone levels.
Pros: Non-invasive, daily dosing flexibility, mimics natural testosterone production
Cons: Transfer risk to partners/children, skin irritation, higher cost ($200-$500 monthly), requires consistent application timing
Testosterone Patch
Transdermal application via adhesive patch worn 22-24 hours daily delivers continuous testosterone absorption.
Pros: Steady hormone levels, convenient
Cons: Skin irritation, visible, moderate cost ($150-$300 monthly)
Testosterone Pellet Implants
Surgical insertion of testosterone pellets under skin (typically buttocks) releases hormones over 3-6 months.
Pros: Long-duration, no daily administration, stable levels
Cons: Minor surgical procedure, difficult dose adjustment, higher upfront cost ($400-$800 per insertion)
Comparison: Testosterone Injections vs Gel Which Is Better
According to clinical data (Journal of Clinical Endocrinology & Metabolism, 2022), both methods achieve therapeutic testosterone levels effectively. Testosterone shots provide superior cost-effectiveness and reliability, while testosterone gels offer convenience and avoid injection anxiety. The best method of testosterone replacement therapy depends on individual preferences, lifestyle, and tolerance.
Step 5: Initiate Your Testosterone Therapy Program and Establish Dosage
Begin your supervised TRT with conservative dosing under medical guidance. Typical starting doses include testosterone cypionate 100-200 mg intramuscularly every 7-14 days, testosterone gel 5-10 grams daily, or equivalent doses for other delivery methods.
Your doctor prescribed testosterone regimen aims to achieve optimal testosterone levels on TRT between 400-800 ng/dL total testosterone and 10-25 ng/dL free testosterone levels. What is a normal testosterone level for men varies by age, but treatment targets mid-normal range.
First 30 days expectations:
- Week 1-2: Initial hormone level changes, possible energy improvement
- Week 3-4: Early symptom relief, increased motivation, better sleep quality
- Week 5-8: Noticeable improvements in libido, muscle recovery, mood stability
- Week 9-12: Continued benefits including body composition changes, strength gains
Track what to expect from testosterone replacement therapy using a symptom journal. How quickly does testosterone replacement therapy work varies individually, but most men report initial improvements within 3-4 weeks with progressive enhancement over 6-12 months.
Step 6: Monitor Testosterone Levels and Adjust Treatment Protocol
Establish regular testosterone monitoring schedule to optimize hormone management and prevent testosterone therapy side effects. Schedule follow-up blood work at 6 weeks, 3 months, 6 months, then every 6-12 months thereafter.
Monitoring protocol:
- Test testosterone levels 48-72 hours after injection (for injectable testosterone) or 4-6 hours after gel application
- Monitor hematocrit and hemoglobin every 3-6 months (TRT can increase red blood cell production)
- Check PSA levels every 6-12 months in men over 40
- Assess estrogen levels if experiencing water retention, gynecomastia, or mood changes
- Evaluate DHT (dihydrotestosterone) if experiencing hair loss or prostate concerns
- Review liver function annually if using oral testosterone
Adjust testosterone dosage based on lab results testosterone and symptom response. Dose optimization typically occurs over 3-6 months to achieve hormonal balance without supraphysiological levels.
Consider consulting specialists at Mens Health Solutions for comprehensive hormone optimization programs that integrate lifestyle modifications with medical grade testosterone therapy.
Troubleshooting Common TRT Issues
If experiencing high estrogen symptoms (water retention, emotional sensitivity, gynecomastia): Request estrogen panel; consider aromatase inhibitor at low dose (0.25-0.5 mg anastrozole twice weekly); reduce testosterone dosage 10-20%.
If testosterone levels remain low despite treatment: Verify proper injection technique; confirm medication quality from pharmaceutical testosterone source; rule out absorption issues; consider switching delivery method; evaluate for underlying pituitary dysfunction.
If developing elevated hematocrit (>54%): Donate blood every 8-12 weeks; increase hydration to 100+ ounces daily; reduce testosterone dose by 10-25%; consider switching from injections to daily gel application; evaluate for sleep apnea.
If experiencing acne or oily skin: Assess DHT levels; use topical treatments; reduce dose slightly; ensure proper skincare routine; consider 5-alpha reductase inhibitor if severe.
If injection site reactions occur: Rotate injection sites; use smaller gauge needles; warm testosterone to room temperature before injection; consider switching to subcutaneous from intramuscular; apply ice pre-injection and heat post-injection.
If energy levels fluctuate dramatically: Switch to more frequent, smaller doses (daily or every-other-day subcutaneous); verify injection timing consistency; assess sleep quality and cortisol levels; evaluate thyroid function.
Next Steps for Long-Term TRT Success
After establishing stable testosterone replacement therapy, focus on maximizing how testosterone replacement therapy improves quality of life through integrated lifestyle optimization:
- Resistance training: Perform strength training 3-4 times weekly to maximize muscle protein synthesis and testosterone utilization
- Optimize nutrition: Consume 1.0-1.2 grams protein per pound bodyweight; maintain healthy fats at 25-30% total calories; support Leydig cells function with zinc (15-30 mg daily) and vitamin D (2000-5000 IU daily)
- Manage stress: Practice stress reduction techniques to prevent cortisol from interfering with testosterone therapy effectiveness
- Prioritize sleep: Achieve 7-9 hours nightly to support hypothalamus and pituitary gland hormone regulation
- Avoid testosterone boosters: Recognize the difference in testosterone replacement therapy vs testosterone boosters—TRT provides pharmaceutical precision versus unregulated supplements
- Consider fertility preservation: If planning children, discuss HCG (human chorionic gonadotropin) co-administration to maintain testicular function and sperm production
- Regular provider communication: Maintain 3-6 month check-ins with your hormone doctor for ongoing testosterone management optimization
Understanding what results can I expect from TRT requires realistic expectations: most men achieve 70-80% symptom improvement with proper hormone restoration, but TRT is not a cure-all. Success depends on proper diagnosis, appropriate treatment selection, consistent monitoring, and lifestyle integration for sustained male vitality and hormonal health.